To understand the regulation and release of stomach acid, we need to know some important type of cells present in stomach and duodenum [First part of small intestine], just after stomach.
Stomach
Parietal cells are located in stomach and releases Gastric acid under direct influence of following factors:
Gastrin is produced by G cells mostly located in stomach which gets signal to release Gastrin under following conditions:
Stomach
- Parietal Cells : Releases Stomach Acid [HCL]
- Chief Cells: Releases Pepsinogen
- EnteroChromaffin Like Cells : Releases Histamine
- G Cells : Releases Gastrin
- S cells : Releases Secretin
Regulation & Release of Stomach Acid
Increases Production Of Stomach Acid
Parietal cells are located in stomach and releases Gastric acid under direct influence of following factors:
- Gastrin
- Acetylcholine
- Histamin
Gastrin is produced by G cells mostly located in stomach which gets signal to release Gastrin under following conditions:
- Distension of Stomach : Most Important factor for the release of Gastrin
- Amino Acids
- Vagal Stimulation : Causes release of Acetylcholine and Gastrin Releasing Peptide [GRP]
Enterochromaffin like cells in stomach releases Histamine which has dual action:
It directly activated Parietal cells to release stomach acid
Potentiates the action of Acetylcholine and Gastrin on parietal cells.
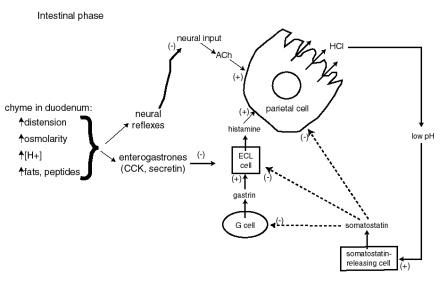 |
| Stomach Acid Release & Regulation © washington.edu |
Decreases Production Of Stomach Acid
Somatostatin : Also known as growth hormone inhibiting hormone [GHIH] acts as a counterbalance for stomach acid release. It is produced in stomach, intestine and Delta cells of pancreas and inhibits acid secretion from parietal cells by three ways:
- Inhibits the release of Histamine
- Inhibits the release of Gastrin
- Directly inhibits Parietal cells and decreases the production of stomach acids
S cells present in duodenum produces Secretin which are activated by presence of acid in small intestine and inhibits the production of Gastrin by G cells thus decreasing acid production by stomach. Secretin also causes release and production of pancreatic as well as biliary bircarbonate
Zollinger Ellison Syndrome is a condition where their is excessive secretion of Gastrin from G cells, which is discussed in detail in separate article



